
More than 40 families whose children died from fentanyl poisoning gathered outside Snapchat’s Santa Monica headquarters on February 12, 2026, painting 108 names onto the pavement in white.
It’s a street memorial to lives claimed by the opioid crisis one counterfeit pill at a time. For the families, this protest isn’t about social media policy. It’s about the deadliest synthetic opioid in American history reaching teenagers through an app on their phones.
The Opioid Crisis by the Numbers
The scale of this tragedy is inseparable from the broader fentanyl epidemic. In 2024, the CDC recorded 79,384 drug overdose deaths in the United States CDC, a significant drop from the peak, but still a staggering toll.
Overall, 2024 saw 27% fewer fatal overdoses across all age groups compared to the deadliest years, and among young people aged 20 to 29, fatal overdose risk dropped by nearly half.
For teenagers specifically, federal data revealed a 40% decline in fatal teen overdoses in 2024, the most encouraging drop in years. But the grief outside Snap’s offices is a reminder of how far we still have to go.
Adolescent overdose deaths in 2023 still stood at more than twice their pre-pandemic level, 708 deaths compared to 282 in 2019. KFF And the social media connection is not abstract.
The National Crime Prevention Council estimates that eight in ten teen and young adult fentanyl overdose deaths are associated with social media contact.
How Counterfeit Pills Are Reaching Teenagers
The pattern behind these deaths is devastatingly consistent. Teens used platforms like Snapchat and TikTok to connect with drug dealers, seeking prescription pills like OxyContin or Percocet. Instead, they received fentanyl, a highly potent synthetic opioid that killed them.
In 2023, seven out of every ten counterfeit opioid pills seized by the Drug Enforcement Administration contained a potentially deadly dose of fentanyl. These teens weren’t seeking hard drugs, most were experimenting with what they believed were ordinary pain pills.
Internal Snap documents cited at the protest revealed that the company internally acknowledged being overwhelmed with issues including sexual extortion, and that it can take under a minute to use Snapchat to arrange an illegal drug purchase.
The advocacy group Heat Initiative also cited claims that 96% of abuse reports submitted through the app go unreviewed by Snap’s Trust and Safety team. Santa Monica Observer
Samuel Chapman, who lost his 16-year-old son after a drug dealer connected with the boy through Snapchat and delivered a fentanyl-laced pill directly to their home, has become a driving force in the movement.
He now leads the Parent Collective and advocates for “Sammy’s Law,” which would require platforms serving minors to use third-party safety software to alert parents to dangerous activities.
Why Fentanyl Is So Deadly for Teens
Fentanyl is a synthetic opioid approximately 100 times more potent than morphine. It is now the primary driver of overdose deaths across virtually every demographic in the United States. Fentanyl is involved in at least 75% of adolescent overdose deaths, and most of those deaths, 84%, are classified as unintentional.
These are not deaths by addiction in the traditional sense. They are poisonings. Many teens had no idea what they were taking.
Adolescent drug use has actually declined in recent years, but the overdose death rate more than doubled between 2019 and 2022, because even a single experimental encounter with a contaminated pill can now be fatal.
Naloxone (brand name Narcan) is an opioid overdose reversal medication that can prevent death if administered quickly. It is available without a prescription at most pharmacies. Every family with a teenager should have it on hand.
The Legal and Policy Battle Over Platform Accountability
The pattern behind these deaths is devastatingly consistent. The February protest coincided with a landmark trial in Los Angeles examining whether social media companies can be held liable for allegedly promoting a harmful product and addicting users. TikTok and Snap settled for undisclosed sums rather than face the trial.
More than 65 families are now part of lawsuits alleging that Snapchat functions as a defective product that facilitates deadly drug transactions.
Snap responded to the protest with a statement. The company condemned the criminal conduct of drug dealers and called for a united response involving law enforcement, government officials, educators and tech companies working together.
The company also noted substantial investments in detection technology and law enforcement cooperation.
Protesters, and many public health advocates, say that is not enough. Families demanded sweeping safety reforms, including defaulting minor accounts to the most private settings, removing addictive features, disabling AI chatbots for young users, and enforcing stricter age verification.
Harm Reduction and Treatment Resources
If someone in your home uses drugs, or you suspect they might, naloxone saves lives. It is available over the counter at CVS, Walgreens and many local pharmacies.
Fentanyl test strips, which can detect fentanyl contamination in pills or powders, are now legal in most states. If you or loved one is need of additional help, you can search Narcotic.com’s list of NA meetings in your area or call 800-934-1582(Sponsored) .

Chris Pielli is a State Representative for Chester County. He has put forward a legislative package aimed at reducing opioid addiction deaths in Pennsylvania caused by fentanyl overdoses.
His proposal calls for the allowance of over-the-counter availability of nalmefene. The FDA has approved the medication for reversing opioid overdoses.
Proposed Changes to Opioid Overdose Laws
Pielli’s House Bill 2181 would amend the state’s Controlled Substance Drug, Device and Cosmetic Act to view nalmefene as an opioid antagonist that’s currently only available via prescription.
A companion measure is House Bill 2182 that would require the Pennsylvania Department of Health to label nalmefene as an opioid reversal agent that doesn’t need a prescription and can be bought without prescriptions.
The Pennsylvania Department of Health currently only approves naloxone as an opioid antagonist, despite nalmefene earning FDA approval in 2023. Many others find refuge and peer support in Narcotics Anonymous (NA Meetings), though prevention and overdose reversal measures are still critical.
Addressing the Opioid Epidemic in Pennsylvania
The Keystone State is no stranger to the weight of the ongoing opioid crisis. Over 4,700 Pennsylvanians died from opioid-related overdoses in 2023, nearly 77% of whom succumbed to fentanyl.
For Pielli, the General Assembly must continue to advance the latest advances in addiction medicine to overcome the high death toll. He describes naloxone as a crucial tool but emphasizes the need for more options as illicit drug markets evolve.
Nalmefene vs. Naloxone for Opioid Overdose
Naloxone and nalmefene are both opioid antagonists that block the effects of opioids and reverse the symptoms of overdose.
The major difference between the two is their half-life durations. This is how long it takes for the concentration of the medicine to drop below one half of the original levels in your bloodstream.
Naloxone has a half-life of 1-1.5 hours so its effects can start to wear off in that time. In contrast, nalmefene has a half-life of nearly 11 hours.
With illicit drugs like synthetic fentanyl constantly increasing in potency and duration, that extra time is vital for preventing secondary overdose after naloxone wears off.
Find Opioid Addiction Support Today
If you or someone you know is at-risk of an opioid overdose, any delay is too long. Call 800-934-1582(Sponsored) or find an NA meeting in Pennsylvania that can support you at no charge.

By 2016, Alabama had the highest number of opioid prescriptions per capita in the nation, fueling rising rates of opioid abuse and fatal overdoses.
The number of fatal overdoses was continuing to escalate. To address the growing opioid addiction crisis, Governor Kay Ivey established a data committee.
Why data? Why not establish more treatment programs? Or education and prevention?
While those efforts continued throughout Alabama, leadership recognized that having better data available could strengthen and guide those other efforts to make them more effective.
How Alabama Tracks Opioid Abuse Data
Alabama’s central data repository (CDR) is funded by the Department of Public Health and overseen by the University of Alabama’s Institute of Data and Analytics.
The CDR pulls opioid abuse data from multiple sources to create a robust source of information for agencies and programs across the state.
Sources include:
- Alabama Department of Mental Health
- Criminal justice data
- Alabama poison information center
- ER, prescription, and opioid-related death data
- State and private health insurance data
- Alabama Department of Public Health’s EMS database
Each agency involved submits data to the CDR, where it is converted and standardized into accessible dashboards that are free to utilize.
How the CDR Strengthens the Opioid Response
Pooling these data sources into a comprehensive set of statistics has provided multiple benefits for the state. It provides a holistic view of the problems and allows establishment of targeted and strategic approaches to address problems
It also gives insight to measure the effectiveness of current programs and keeps the public and stakeholders informed of current opioid abuse and overdose trends.
Additionally, it establishes communication between otherwise isolated agencies. Officials can use CDR data to apply for funding for opioid-related programs.
For example, if data reveals that overdoses are higher in one county, officials can target treatment programs for that area, then monitor the data to see if the new efforts make an impact.
Can Other States Replicate Alabama’s Opioid Strategy?
While the number of opioid overdoses has decreased in recent years, thousands of people across the nation continue to experience fatal overdoses each month. As state officials look for solutions, they can model Alabama’s data-driven approach.
Based on lessons learned from the establishment and execution of the CDR, Alabama’s data experts recommend several key steps to success:
- Make data-sharing as simple and easy as possible for contributors
- Cast a wide net for data contributors
- Demonstrate tangible benefits for contributors
- Develop a strategic plan to ensure data is sharable, usable, and frequently updated
As Alabama officials have discovered, this process provides a powerful network of data that can strengthen efforts, enhance programs, and save lives.
Finding Opioid Addiction Support
If you or a loved one is struggling with opioid use, there support options available. Search through Narcotics.com’s directories for local Narcotics Anonymous meetings near you or call 800-934-1582(Sponsored) today for immediate guidance.

If you think the opioid epidemic is only a problem for younger generations, think again. Adults 65 and older are facing growing risks as senior opioid overdose deaths continue to rise. According to a recent study, fatal overdoses among seniors increased by 9% in just the last eight years. The majority of fatalities stemmed from the dangerous cocktail of fentanyl combined with stimulants.
The research was presented at the ANESTHESIOLOGY annual meeting and used data from the Centers for Disease Control and Prevention (CDC). Seniors are frequently overlooked when it comes to opioid studies and yet they’re part of the rising surge of drug overdoses taking lives across the nation.
Why Seniors Are at Higher Risk
Why are these groups more vulnerable to opioid overdose events? One reason is that many of them may already have chronic health conditions that affect them. The epidemic has happened in stages, with the beginning being prescription medications in the 1990s. Then came heroin, fentanyl, and now, fentanyl mixed with stimulants such as cocaine. This fourth phase is where older adults have been impacted most.
Over 400,000 death certificates were analyzed between 2013 and 2023 for the study. All of them listed fentanyl as the cause of death. The rise in fentanyl related overdoses among seniors seemed to start in 2015 and saw a noticeable spike in 2020.
How to Prevent Senior Opioid Overdoses
The study illustrates many findings, including the incidence of drug sharing among older adults, the need for improved patient monitoring when prescribing opioids, adjusting perioperative planning for this age group, and using clear labeling practices.
Although the trends are daunting, there are still steps within our control that may help decrease the chances of these occurrences. Knowing this group is also vulnerable can shine a light on the need for education and proper maintenance for prescriptions. One of the goals is to minimize the use of this drug as a pain control method and to look for safer ways to treat older adults.
If you or a senior you love is struggling with opioid addiction, support is available.
Find local Narcotics Anonymous meetings or senior focused recovery programs in your area or call 800-934-1582(Sponsored) for immediate assistance.

Tracy was aiming for a vein, but she missed. Instead of entering her bloodstream, the heroin went directly into the fatty tissue around the vein. It hurt, but she figured it was no big deal.
She was wrong…
4 Dangers of Missing the Vein With IV Drug Use
 Injecting a drug (often called “shooting up”) means using a needle to deliver drugs like heroin, cocaine, and methamphetamine directly into a vein. When the needle fails to reach its target, this is called a “missed shot.”
Injecting a drug (often called “shooting up”) means using a needle to deliver drugs like heroin, cocaine, and methamphetamine directly into a vein. When the needle fails to reach its target, this is called a “missed shot.”
A “missed shot” happens when a needle either: 1) doesn’t enter the vein properly, 2) enters the vein then slips out again, or 3) enters the vein and goes all the way through to the opposite side of the vein.
During IV drug use, when the needle slips or punctures the vein, it causes fluid to enter the tissue around the injection site. This often leads to infection, and from there, things can quickly go downhill. People can experience abscesses, cellulitis, vein collapse, and other complications.
Let’s take a look at four serious problems that can develop if IV drug users miss the vein.
#1 Abscesses
When a missed shot gets infected, you may get an abscess at the injection site. Your body is trying to fight the infection, so it sends cells to the damaged tissue to repair it. This causes the area to become swollen and fill with pus. (Pus is a mix of white blood cells that are sent to fight the infection, plus germs and dead tissue.)
Side effects of an abscess include:
- Redness of the skin
- Smooth swelling under the skin
- Pain in the infected area
- Warmth of the skin in that area
- A build-up of pus in the area
Because of the infection, you may also experience a fever and chills. Here’s how some people have described the abscess experience:
“It gets red, and it gets hot, and it hurts. It gets to a point when you just can’t bear it any more. You just can’t walk. Or you can’t use wherever it is on your body, you can’t use that limb. You can’t use your arm. You can’t use your leg or your foot. It becomes to where it’s like affecting you and you can’t function.” ~ 37-year-old woman
#2 Cellulitis
A missed shot can also lead to cellulitis. This is a deep, bacterial skin infection. It can occur when a break in the skin allows bacteria to invade (which happens when drugs are injected outside a vein). And it can be very serious.
Common symptoms of cellulitis include:
- Pain
- Tenderness
- Swollen skin
- Redness of the skin
- Bruising
- Blisters
- Fever
- Headache
- Weakness
- Chills
The pain and other symptoms start at the injection site, but the infection can spread quickly throughout the body. It can cause damage to tissue and tissue death. If you get cellulitis repeatedly, this can cause damage to your lymphatic drainage system and cause ongoing swelling of the affected arm or leg.
And the infection can enter your bloodstream, lymph nodes, bones, heart, or nervous system. At that point, it can become life-threatening. Complications from cellulitis can lead to amputation or even death. When you factor in the complications from addiction, it’s easy to see how things can spiral.
#3 Vein Collapse
Repeated missed shots can also cause your veins to collapse.
Here’s how it happens:
- The injection causes damage to the lining of the vein.
- Clots form around the damaged site.
- The clots harden into scar tissue.
- These clots narrow the vein, which restricts blood flow and causes future clots to form more quickly.
- Eventually, the sides of the vein heal together (the vein “collapses.). There’s so much scar tissue that it draws the sides together and shuts off the vein.
Once a vein collapses, blood can no longer flow through it. Sometimes a collapsed vein can heal, but the damage can be severe enough that the collapse is permanent. In some cases, this can cause circulation problems.
#4 Substance Complications
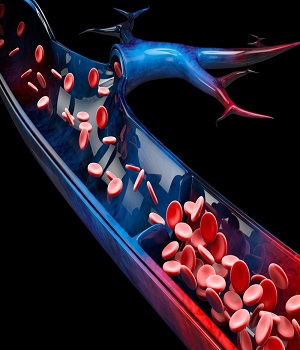 In addition to the damage caused by the needle, the drugs themselves can irritate the vein or cause other issues. For example, research has shown that the acidity in heroin can damage veins. Researchers found that some batches of heroin have a pH level as low as 2.6 – which means the heroin is very acidic. (In comparison, lemon juice and vinegar both have a pH of 2.) Imagine the irritation your veins would experience with something that acidic flowing through them. With repeated exposure to such high pH levels, veins can develop life-threatening infections.
In addition to the damage caused by the needle, the drugs themselves can irritate the vein or cause other issues. For example, research has shown that the acidity in heroin can damage veins. Researchers found that some batches of heroin have a pH level as low as 2.6 – which means the heroin is very acidic. (In comparison, lemon juice and vinegar both have a pH of 2.) Imagine the irritation your veins would experience with something that acidic flowing through them. With repeated exposure to such high pH levels, veins can develop life-threatening infections.
It’s also worth mentioning that, when people inject heroin that is mixed with cocaine, the cocaine actually numbs the injection area. That means you aren’t able to feel the typical pain associated with missing the vein. And when you can’t feel it, you don’t know there’s a problem.
IV Drug Users Can Expect Complications
Are complications from missed shots a common problem? Are you likely to experience one of these issues? Well, over half (56%) of people who inject drugs admit they’ve missed a vein. And one in six intravenous drug users reports experiencing a missed shot more than four times every month.
So, yes, IV drug use problems are common, and the risks are high.
 You may know him as a young John Conner in Terminator 3: Rise of the Machines. Or you may recognize him as the child actor who co-starred with Mel Gibson in Man Without a Face in 1993.
You may know him as a young John Conner in Terminator 3: Rise of the Machines. Or you may recognize him as the child actor who co-starred with Mel Gibson in Man Without a Face in 1993.
Nick Stahl began performing at age 4 and was recruited by Hollywood at age 10. He was just 11 when Gibson discovered Nick’s talent, and his career took off from there.
And it was just two years later, at age 13, that Stahl discovered alcohol.
But let’s back up a bit.
Looking back at his childhood, Stahl gains some insight into why the stage was so appealing – and why alcohol was so appealing at a young age, too.
A Blanket of Fear
 Stahl was raised by a single mom who worked two jobs to make ends meet.
Stahl was raised by a single mom who worked two jobs to make ends meet.
Stahl recalls, “From a very young age, I was always under this blanket of fear, financial fear. There was this idea that if we didn’t come up with enough money for that month, we would end up on the street. That colored my outlook growing up. My default mode was untrusting, with this mentality of waiting for the other shoe to drop.”
“I don’t look back on my childhood with real fond memories,” he says. “But for some reason, when I did plays, that stuff shut off and I had this ability to just be very comfortable.”
And when he had his first drink at 13, he discovered a way to “shut stuff off” when he wasn’t on stage. The tense feelings disappeared.
“Suddenly, I had a freedom from thinking, from uncomfortability,” he explains. “I felt okay in my skin — and I hadn’t really felt that before.”
Full Steam Ahead
By age 16, Stahl’s career was in full gear, and he and his mother moved to Los Angeles. There, he discovered the party scene.
He recalls, “I was going to bars. I had a very easy time getting into these places. A lot of my friends were older, and I had a great time.”
It wasn’t long before he was smoking weed. And from there, he moved on to pills, cocaine, and meth.
“That became what I chased,” he says. For Stahl, the drugs alleviated anxiety. He wasn’t partying for fun, but for release. He explains, “Very early on, it was not ‘I want this,’ but ‘I need this.’”
Falling Apart
In 2001, Stahl starred in Bully, a true-crime drama. Brad Renfro, his co-star, also battled addiction at the time.
Stahl recalls, “He was more severe in his addiction than I was. He just progressed to a point where he had to have someone on set with him to keep him sober.”
Stahl knew he was headed in the same direction. He tried to stop the deadly addiction train he was on.
“Throughout my 20s, I experimented with different ways to regulate my drinking. Maybe LA is the issue, right? So, I’d move. Maybe these certain friends I’m hanging out with, maybe that’s the issue. So, I’d get new friends.”
But none of that worked.
“Things started to get awful pretty quickly,” Stahl recalls. “I started to miss appointments. I put on a good front. The extent of my illness stayed hidden even from me. It’s common to justify, rationalize things. I looked around and said, ‘Everyone is partying the way I am.’ In retrospect, there were far less people going as hard as I did.”
In 2007, at age 27, Stahl entered rehab for the first time. In 2009, he tried again.
After two failed attempts at recovering from addiction in LA, Stahl moved back to his home state of Texas.
But Stahl couldn’t stay away from Hollywood for long. He went back – and was arrested multiple times. The charges included disorderly conduct and possession of meth.
Picking Up the Pieces in Recovering from Addiction
Despite his struggles, Stahl never lost an acting job. He was able to hold it together enough that he never got fired. But he knew he would soon, if something didn’t change. In 2012, he knew it was time to step away from acting for a while.
“I was physically there, but I was checked out,” he admits, “and I certainly wasn’t feeling any real enthusiasm for acting anymore. I knew that I had to step away, for self-preservation, but also for the preservation of my career, if I was going to have one again.”
Stahl spent the next five years in Dallas, “diving into his recovery” as he puts it.
“I didn’t think it would be easy, but it proved to be even more difficult than I thought it would be,” he says. “It’s hard to put my finger on what shifted. If I hit bumps in the road, I always got up and tried again. Luckily, I was resilient…One day, it just kind of stuck.”
Once he achieved sobriety, Stahl was able to give his life new direction. “It proved to be reconstructive for me,” he says. “That’s when I really started to piece together that I had neglected building a real life outside of the business. For many years, I had everything — but I didn’t have anything resembling a satisfying life. I didn’t have outside interests, I lost touch with friends and family. The film world made up too much of my identity.”
A New Life While Recovering from Addiction
When Stahl stepped away from Hollywood while recovering from addiction, he didn’t leave with millions in the bank. That meant he had to get a job like any other Joe. “So, I started working for a friend’s moving company,” he says.
 “I tried other things. I worked at a coffee shop in New York for a little bit. Not only did I learn how to live as a sober person, which I didn’t know how to do, but I learned how to have a life outside the business.”
“I tried other things. I worked at a coffee shop in New York for a little bit. Not only did I learn how to live as a sober person, which I didn’t know how to do, but I learned how to have a life outside the business.”
And this fresh perspective has allowed Stahl to re-enter show business with a healthy, sober outlook. “That passion inside me that burned for film and acting, it had dulled progressively over time,” he explains.
“But once I was separated from Hollywood, all of that started to come back. Over the past few years, whether I’m working on a film or auditioning, I don’t take it for granted, ever. I work much harder at it now. I just feel a renewed love for it.”
Clean for four years now, Stahl, age 41, is back in action with a full line-up of acting roles on his calendar.
But recovering from addiction comes first. “Recovery has to be the most important thing for me,” he says. “I put it first in my life. But I’m grateful for it, and it’s given me the opportunity to try to help people in the same situation I was [in]. It’s more important to me than making films. I search out people who have had similar struggles and show them how I got well. I speak from my experience and show them what worked for me.”
If you or someone you love is experiencing a substance use disorder, help is available. Call 800-934-1582(Sponsored) today.
You say tomato. I say tomahto.
You say oxycodone. I say Percocet. Same difference, right?
Actually, no. The two drugs do have some similarities, but when comparing opioids, the terms are not interchangeable.
Let’s talk about how they differ.
Chemical Makeup
 Both of these drugs are opioid pain medications. Oxycodone is a synthetic drug made from opium. Percocet is made of oxycodone and acetaminophen. (Acetaminophen is another painkiller, which you probably know by its brand name: Tylenol.)
Both of these drugs are opioid pain medications. Oxycodone is a synthetic drug made from opium. Percocet is made of oxycodone and acetaminophen. (Acetaminophen is another painkiller, which you probably know by its brand name: Tylenol.)
If you take either of these drugs, you’re taking oxycodone. But when you take Percocet, you’re also getting the second medication, acetaminophen. This is one of the primary reasons oxycodone and Percocet get confused when comparing opioids.
Oxycodone is a generic drug, which is sold under several brand names. Percocet is one if the brand name drugs made with oxycodone.
Oxycodone and Percocet Use
Oxycodone is available in three different forms, which are used for different types of treatment:
- Immediate-release tablets enter the bloodstream right away
- Extended-release tablets gradually release the drug into the bloodstream
- An oral solution, often given through a gastric tube, is available for patients who can’t swallow tablets
Oxycodone is used for treating moderate to severe pain. The extended-release form is often prescribed for patients who have ongoing pain, such as cancer-related issues.
Percocet is also prescribed to treat moderate to severe pain. But it is used for treating conditions that also cause a fever because acetaminophen is a fever reducer. It may also be used to treat patients who experience pain while on another long-acting painkiller.
Percocet is not recommended for long-term use, since the acetaminophen in it can wreak havoc on the liver and cause serious damage over time.
Effectiveness
Both drugs are proven to effectively relieve pain. When you take Percocet or immediate-release oxycodone, you start to feel relief within half an hour, and the effects usually last for three to six hours.
Extended-release oxycodone starts to work within two hours and continues to relieve pain for up to 12 hours. The brand name drug OxyContin is a type of extended-release oxycodone.
Over time, patients can develop tolerance to these drugs. This means they need higher doses to get the same pain relief. Tolerance can begin to develop within just one week of taking regular doses of either drug.
Side Effects
Since we’re comparing opioids with the same primary ingredient, both oxycodone and Percocet naturally have similar side effects.
Both commonly cause:
- Constipation
- Sleepiness
- Calmness
- Nausea
- Dizziness
- Loss of appetite
- Headache
- Impaired motor skills
There are two main differences in their side effects:
- Oxycodone is more likely to cause feelings of euphoria
- Percocet can cause abdominal pain, black stools, and yellowing of the skin (jaundice) because of its effect on the liver
One of the biggest potential side effects of either drug is addiction. Tolerance can happen quickly and lead to physical and psychological dependence, so “>both drugs are considered highly addictive.
Drug Classification
Here’s an area where the two drugs don’t differ. The Drug Enforcement Administration (DEA) classifies drugs into five categories or “schedules.” A drug’s class is determined by its potential for dependency and its accepted medical use.
Both oxycodone and Percocet are Schedule II drugs.
Schedule II substances have “a high potential for abuse, with use potentially leading to severe psychological or physical dependence.” They are considered dangerous.
Other examples of Schedule II drugs include methamphetamine, cocaine, fentanyl, and Ritalin.
Pop Quiz
 Here’s a quick quiz comparing oxycodone and Percocet. Don’t worry – you won’t be graded!
Here’s a quick quiz comparing oxycodone and Percocet. Don’t worry – you won’t be graded!
Match the following descriptions with the correct drug. (Hint: Some are true for both substances.)
- An opioid
- Contains acetaminophen
- Relieves pain
- Is considered addictive
- Comes in an extended-release form
- Can cause drowsiness
- Reduces fever
- Is not recommended for long-term use
- Tolerance can develop in 7 days
- A Schedule II narcotic
How’d you do? You can check your answers below.
And remember, if you’re trying to decide which medication is best for your situation, always consult with a doctor and use the drug only as prescribed.
If you need help with drug abuse, call 800-934-1582(Sponsored) .
Pop Quiz Answers:
- Both
- Percocet
- Both
- Both
- Oxycodone
- Both
- Percocet
- Percocet
- Both
- Both
 Eight days ago, Angela was in rehab. Now she’s completely off heroin and has an impressive five weeks of sobriety under her belt. She has a new job and a new apartment. But things are starting to get a little more stressful than she thought they’d be — so many changes, so many new responsibilities.
Eight days ago, Angela was in rehab. Now she’s completely off heroin and has an impressive five weeks of sobriety under her belt. She has a new job and a new apartment. But things are starting to get a little more stressful than she thought they’d be — so many changes, so many new responsibilities.
One night after work, Angela’s stress became too much to handle. She could feel herself slipping. Her mind was overcome by cravings.
In an instant, that familiar voice in her head reappeared. “You just need a little something to take the edge off — something to help you relax. It’s just this one time. No big deal. You can go back to being sober tomorrow.”
Three hours later, Angela woke up in a hospital bed. She’d overdosed on heroin. Fortunately for Angela, she was saved when a neighbor found her unconscious and barely breathing in their apartment complex hallway. EMTs were able to revive her from the overdose.
Many others aren’t so lucky.
The Heightened Risk of an Overdose After Rehab
 When Angela entered rehab, she stopped using opioids. Before rehab, she had been using drugs for two years. During those two years, her body built up a tolerance for opioids. Eventually, she needed a much bigger dose to keep getting the same effect from the drugs.
When Angela entered rehab, she stopped using opioids. Before rehab, she had been using drugs for two years. During those two years, her body built up a tolerance for opioids. Eventually, she needed a much bigger dose to keep getting the same effect from the drugs.
Fresh out of rehab, Angela had been drug-free for weeks. Her body had returned to a normal, healthy state. And that can be dangerous.
Angela’s systems weren’t constantly interacting with and reacting to the effects of opioids. That means she no longer had the same tolerance she’d built up before entering treatment.
But Angela wasn’t thinking about detox, tolerance levels, or the potential of an overdose. So, she took the same dose of heroin she was using right before rehab. And her body went into shock.
She hit her body with an amount of heroin it was no longer used to, and her system couldn’t handle it. So, it started shutting down.
The result: an overdose that nearly killed her.
The Common Story of Overdosing After Rehab
Angela’s situation isn’t unusual. After leaving rehab, many people return to their old habits. And while their habits haven’t changed, their bodies and tolerance levels have.
When people relapse after treatment, they often make the mistake of thinking they can take the same dose they used pre-rehab. They don’t realize that dose could now be fatal, and they end up overdosing.
Some people get lucky and survive the overdose. But many don’t.
Top Reasons for a Post-Rehab Overdose
Angela looked to opioids to help her cope with stress. This is a common reason for overdose after rehab. Whether at home or work, stress builds up, and the person who is addicted feels they can’t cope with everything without using substances.
Here are five other common mindsets that can lead to a post-rehab overdose:
- Just One More Time:
Jeff wanted to take his life in a new direction. He hadn’t taken any pills in weeks.
But, when he ran into an old friend who invited him over, he knew what they would end up doing. “Why not?” he thought. “I might never see him again. One last time can’t hurt.”
But, yes, it can. Jeff no longer has the tolerance for the level of drugs he and his friend used to use. If he takes that amount tonight, there’s a very good chance he’ll overdose.
- Feeling the pain
Devan’s old shoulder injury was flaring up again. After battling with a painkiller addiction, he had been drug-free for six months. But the pain was back.
And he didn’t think he could manage it without those pills.
The problem: If Devan took the same dose of painkillers today that he was taking when he quit six months ago, the amount would kill him.
- Too Strong for Triggers
Sam used to get high every time he went to his cousin’s house. Now, he’s been out of rehab for three weeks and has stayed clean.
But just walking by his cousin’s place makes him want to use. He doesn’t try to avoid the neighborhood — or his cousin.
And the cravings are getting more intense.
If Sam doesn’t find a way to address his triggers and cravings, and gives in to them, he’ll be in danger of an overdose.
- Something Completely Different
Kelly went to rehab to deal with her alcohol addiction. Three months sober, Kelly starts using heroin instead of drinking. But her body isn’t used to this drug.
Because she substitutes one drug for another, Kelly is at high risk for an overdose.
- Feeling Despair
Sobriety has just become too much. Brian is in a deep well of depression and sees no hope.
He decides to take every pill he can find to escape it all with an intentional overdose to end his life.
And the Leading Cause for an Overdose After Rehab…
 Of all the reasons for post-rehab overdose, one of the most common is self-deception. Here’s what that looks like:
Of all the reasons for post-rehab overdose, one of the most common is self-deception. Here’s what that looks like:
“Sure, I had a drug addiction before, but I have control now. This time, I won’t let things get out of hand.”
But this line of thinking shows that things are already out of hand. And a relapse could be (and often is) fatal — especially after rehab.
For information about treatment options for you or a loved one, call 800-934-1582(Sponsored) today.

– DEA Administrator Anne Milgram
The chemicals come from China to Mexico. The cartels in Mexico run drug production facilities. They sell deadly, unregulated substances, like fentanyl, on social media in the United States. Thousands of Americans die of drug overdose.
The Emerging Risk of Fentanyl on Social Media
 Between April of 2020 and April of 2021, 100,000 Americans died from drug overdose. Around 75,000 of those deaths were due to opioids, mostly fentanyl.
Between April of 2020 and April of 2021, 100,000 Americans died from drug overdose. Around 75,000 of those deaths were due to opioids, mostly fentanyl.
According to data from Families Against Fentanyl, “the number of deaths from fentanyl between 2020 and 2021 surpassed the number of deaths from suicide, COVID-19, and car accidents.”
Fentanyl is a synthetic opioid originally developed to treat severe pain, specifically breakthrough pain in cancer patients. It is 50 -100 times more powerful than morphine.
Like other opioids, fentanyl overdose causes breathing to stop, which can lead to a coma, brain damage, and death.
The U.S. Drug Enforcement Agency (DEA) has confiscated so many pills containing deadly amounts fentanyl that they’ve issued a public safety alert. The pills are made to look like common drugs such as OxyContin, Xanax, and Adderall.
At least 76 recent fentanyl cases involved the use of social media to traffic the drugs. Dealers use Facebook, TikTok, Snapchat, Instagram, and YouTube to reach customers.
DEA Administrator Anne Milgram says:
Why Fentanyl on Social Media is Overtaking the Market
Fake prescription pills laced with fentanyl look nearly identical to legitimate pills. They closely resemble medications like Vicodin, Xanax, and Percocet.
The DEA reports that people use social media to purchase pills that they think are legit, but the pills can turn out to be deadly. Rather than the medication they were expecting, social media buyers receive fakes containing lethal amounts of fentanyl.
And it’s not just teens, either.
Milgram notes that the drug dealers’ social media strategy is “reaching all age groups—a curious teenager ordering a pill online, a college student trying a pill from a friend, an elderly neighbor searching online for a painkiller.”
She says, “They are using these platforms to flood our country with fentanyl. The ease with which drug dealers can operate on social media and other popular smartphone apps is fueling our nation’s unprecedented overdose epidemic.”
What Can Be Done About Fentanyl on Social Media
 The DEA reports that dealers are use emojis as codes to advertise substances like fentanyl on social media. And Milgram says “social media companies are not doing nearly enough to block the ads for fake pills.”
The DEA reports that dealers are use emojis as codes to advertise substances like fentanyl on social media. And Milgram says “social media companies are not doing nearly enough to block the ads for fake pills.”
Social Media Moderation
Social media companies claim they have tried. They say they have altered algorithms and hired more moderators to look for illegal items for sale.
But law enforcement and families of overdose victims say it’s inadequate. They suggest more parental controls and data-sharing to catch dealers who sell drugs like fentanyl on multiple social media platforms. In many cases, the dealer connects with a buyer on one site but goes to another to complete the deal, and then moves to a third to receive payment.
Decreased Social Media Use
Some suggest a radical idea: Don’t use social media. Block it on kids’ phones. Take their devices away. Many generations have survived without social media. Maybe a step back is what it will take to ensure the next one survives, too.
Safe Prescription Use
Meanwhile, the DEA and other law enforcement officials continue their efforts to get fentanyl off the streets and off social media. The DEA offers the following reminder:
“The only safe prescription medications are prescribed by trusted medical professionals, given by a licensed pharmacist. ‘Prescription drugs’ acquired from other sources should be assumed unsafe.”
If you or a loved one misuses prescription drugs, receiving treatment can be crucial. Many people begin using legitimate pills, but develop a high tolerance that requires more pills than are in their prescription to achieve the same effects. This progression can lead into the purchase of potentially dangerous counterfeit prescription pills online, such as fentanyl on social media.
Call 800-934-1582(Sponsored) to learn more about opioids misuse and addiction treatment.

We know addiction can develop from a number of factors. And we also know the experiences we have during childhood can play a role in who we become as adults.
One of the childhood experiences that can have a huge impact on us as we grow older is emotional neglect. In fact, research shows it can even put us at higher risk for developing an addiction.
What is Emotional Neglect?
 Childhood emotional neglect can occur when parents neglect their children’s emotions and emotional needs.
Childhood emotional neglect can occur when parents neglect their children’s emotions and emotional needs.
This means they do not ask about their children’s feelings, connect with them on an emotional level, or validate their feelings enough.
These parents may be physically present but emotionally unavailable, or they could be so damaged by their own childhood experiences of emotional neglect that they have no idea how to nurture their own children.
Emotional neglect is a form of abuse. Emotional neglect is more difficult to spot than physical abuse, but can be just as damaging.
Who are Emotionally Neglectful Parents?
Jonice Webb describes childhood emotional neglect in more detail in a recent Psychology Today article.
Webb states:
The one failure of the emotionally neglected family is emotional. There may be enough hugs. There may be enough money. There may be enough food and clothing. But this family does not manage to provide enough emotional awareness, validation, compassion, or emotional care to the children.
Emotionally neglectful parents usually do not notice what their kids are feeling and, therefore, may have no idea that they’re neglecting their children’s emotions at all.
Connecting the Dots Between Emotional Neglect and Addiction
It is not uncommon for a person in addiction treatment to have an ah-ha moment where they realize their emotional or physical needs were neglected as children. They see for the first time how this neglect influenced their choices, feelings, and behavior as adults.
Researchers acknowledge that it’s impossible to identify the exact role of emotional neglect and other forms of abuse play in addiction. Dr. Cora Lee Wetherington, the National Institute on Drug Abuse’s Women’s Health Coordinator says:
The sheer weight of the many reports over the years certainly implicates child abuses as a possible factor in drug abuse for many people, but we lack hard data that clearly establish and describe the role of child abuse in the subsequent development of drug abuse. Is child abuse indeed a cause of drug abuse, or is child abuse a marker for other unidentified factors?
Emotional neglect and abuse causes:
- Persistent feelings of fear and a high risk of developing post-traumatic stress disorder (PTSD)
- Hypervigilance
- High risk of developing anxiety or depression
- Learning deficits
- Delayed developmental milestones
- Difficulty processing positive feedback
- Difficulty with social cues and situations
These effects also have a high correlation with addiction. For example, research indicates that 30-59 percent of women in treatment for addiction have PTSD and 55-99 percent of these women have a history of childhood trauma, such as physical or emotional neglect.
What Are the Signs of Emotional Neglect?
Webb identifies eight signs of emotional neglect in a family:
- Family conversations tend to focus on surface-level topics, meaning they are seldom about emotional, meaningful, painful, or negative things.
- You sometimes feel unexplained resentment or anger towards your parents.
- You go to family events with hopes of having a good time, but oftentimes, you come away feeling empty or disappointed.
- Interpersonal problems in the family are generally ignored instead of acknowledged and discussed.
- It feels like your siblings are competing with each other, but you’re not sure for what.
- Affection in your family is expressed through acts of service (i.e., doing things for people) and not through emotional expression.
- Emotion, in general, seems to be off-limits in your family.
- When you’re with your family, you feel lonely or left out.
If you identify with any of the above signs, here’s the good news: The way you were raised does not have to dictate the rest of your life.
Can You Repair the Effects of Emotional Neglect?
 While you cannot change the family you were born into, you can start by working on yourself, according to Webb. She recommends selecting an item from the list that applies to your family, and then to start behaving the opposite way.
While you cannot change the family you were born into, you can start by working on yourself, according to Webb. She recommends selecting an item from the list that applies to your family, and then to start behaving the opposite way.
Webb also recommends making an effort to:
- Talking to others about meaningful things instead of only talking about superficial things
- Fighting against feeling guilty for your emotions
- Focusing on self-care when with your family
- Expressing your affection and warmth toward others through words, rather than actions
By taking these first steps, you will be better able to offset the impact the emotional neglect you experienced will have on your life moving forward.
Call 800-934-1582(Sponsored) today to learn more about treatment options.
